Helping The others Realize The Advantages Of Impedance Tomography
Helping The others Realize The Advantages Of Impedance Tomography


Electrical Impedance Tomography for Cardio-Pulmonary Monitoring
Abstract
Electrical Impedance Tomography (EIT) is an instrument used to monitor the bed that noninvasively visualizes local ventilation as well as conceivably lung perfusion distribution. The present article reviews and analyzes both methodological and clinical aspects of thoracic EIT. Initially, researchers were concerned about the validation of EIT for measuring regional airflow. These studies focus on its clinical applications to determine the extent of lung collapse, the tidal response, and lung overdistension in order to regulate positive end-expiratory pressure (PEEP) and tidal volume. In addition, EIT may help to detect pneumothorax. Recent studies examined EIT as a method to measure lung perfusion in the region. The absence of indicators in EIT measurements could be adequate to continuously measure cardiac stroke volume. Utilizing a contrast agent, such as saline, may be required to measure regional lung perfusion. Thus, EIT-based monitoring of respiratory ventilation and lung perfusion can reveal the perfusion match and local ventilation and can prove helpful in the treatment of patients suffering from acute respiratory distress syndrome (ARDS).
Keywords: electrical impedance tomography Bioimpedance; image reconstruction Thorax; regional adrenergic and regional perfusion monitoring.
1. Introduction
The electrical impedance imaging (EIT) is an radiation-free functional imaging modality that allows non-invasive bedside monitoring of regional lung ventilation and arguably perfusion. Commercially available EIT devices were developed for the clinical use of this technique and the thoracic EIT has been successfully used for both pediatric and adult patients 1, 1.
2. Basics of Impedance Spectroscopy
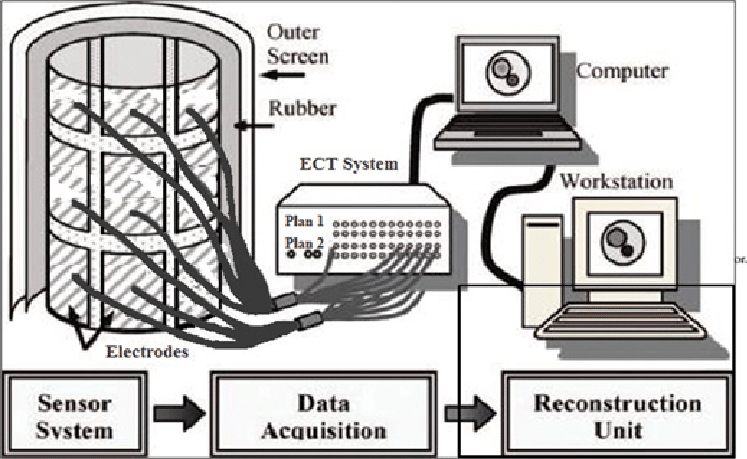
Impedance Spectroscopy may be described as the resistance of biological tissues to externally applied alternating voltage (AC). It is usually measured with four electrodes, of which two are used to inject AC injection, and the remaining two for voltage measurement 3,,3. Thoracic EIT measures the regional range of intra-thoracic bioimpedance. This can be considered like an extension of principle of four electrodes to the imaging plane, which is divided through the electro belt [ 1]. Dimensionallyspeaking, electrical impedance (Z) is the same as resistance , and the corresponding International System of Units (SI) unit is Ohm (O). It is easily expressed as a complex number where the real portion is resistance and the imaginary is known as reactance, which determines the effect of an inductance, capacitance, or. Capacitance is dependent on biomembranes’ specifics of the tissues such as ion channel, fatty acids, and gap junctions. The resistance is primarily determined by composition and the amount of extracellular fluid 1., 22. At frequencies less than 5 Kilohertz (kHz), electrical current runs through extracellular fluid and is heavily dependent on the characteristics of resistivity of tissues. In higher frequencies above 50 kHz, electrical currents can be slightly deflected through cell membranes , which results in an increase of capacitive tissue properties. When frequencies exceed 100kHz the electrical current is able to pass through cell membranes, reducing the capacitive component [ 21. Therefore, the effects which determine the level of impedance in the tissue depend on the utilized stimulation frequency. Impedance Spectroscopy is typically described as conductivity or resistance. Both regulates conductance or resistance according to the area of the unit and the length. The SI units for the same include Ohm-meter (O*m) for resistivity and Siemens per meters (S/m) to measure conductivity. Resistivity of thoracic tissue ranges from 150 o*cm for blood to 700 O*cm when it comes to lung tissue that has been deflated, and up to 2400 O*cm in the lung tissue that has been inflated ( Table 1). In general, tissue resistance or conductivity is dependent on volume of the fluid and the amount of ions. Regarding the lungs, it also is dependent on the quantity of air inside the alveoli. Though most tissues exhibit an isotropic characteristic, the heart and the muscles in skeletal tend to be anisotropic, which means that resistance strongly depends on the direction that you measure it.
Table 1. Electrical resistance of thoracic tissues.
3. EIT Measurements and Image Reconstruction
In order to conduct EIT measurements, electrodes are placed around the thorax in a transverse plan that is usually located in the 4th to 5th intercostal spaces (ICS) in an angle called the parasternal line5. Subsequently, the changes of impedance are measured in those lobes that are lower in the left and right lungs and also in the area of the heart ,2[ 1,2]. To position the electrodes above the 6th ICS might be difficult as abdominal content and the diaphragm occasionally enter the measurement area.
Electrodes are either single self-adhesive electrodes (e.g., electrocardiogram ECG,) that are placed individually with equal spacing between the electrodes, or are integrated into electrode belts [ ,22. Self-adhesive lines are accessible for a more convenient application ,21. Chest tubes, chest wounds bandsages that are not conductive or sutures made of wire can severely affect EIT measurements. Commercially available EIT equipment typically uses 16 electrodes, but EIT systems with eight and 32 electrodes are available (please look at Table 2 for details) For more information, refer to Table 2. ,21 2.
Table 2. Electric impedance (EIT) tools.
During an EIT measurements, small AC (e.g. approximately 5 milliamps at a frequency of 100 kHz) is applied through various electrode pairs, and the resulting voltages are measured using the other electrodes 6. Bioelectrical impedance that is measured between the injecting and the measuring electrode pairs is calculated using the applied current and measured voltages. Most often nearby electrode pairs are utilized to allow AC application in a 16-elektrode system however 32-elektrode systems usually utilize a skip-pattern (see the table 2) for increasing the spacing between the electrodes for current injection. The resultant voltages are measured by using the remaining electrodes. There is currently an ongoing debate about the various kinds of current stimulation, as well as their specific advantages and disadvantages [7]. To get a complete EIT data set of bioelectrical measurements that are injected and electrode pairs that measure are continually rotating around the entire thorax .
1. Voltage measurements and current application around the thorax using an EIT system with 16 electrodes. Within milliseconds, all the active voltage electrodes and those with active voltage electrodes are continuously rotating across the upper thorax.
The AC that is used in EIT tests is safe to use for use on body surfaces that is undetectable by the patient. For safety reasons, the use of EIT in patients with electrically active devices (e.g., cardiac pacemakers or cardioverter-defibrillators) is not recommended.
This EIT data set recorded over a single cycle that is recorded during one cycle of AC application is referred to as a frame . It is comprised of the voltage measurements necessary to create the image. EIT image. Frame rate refers to the amount of EIT frames recorded each second. Frame rates of no less than 10 images/s is required for monitoring ventilation and 25 images/s to monitor cardiac function or perfusion. Commercially accessible EIT equipment uses frames with a frame rate between 40 and 50 images/s, as depicted in
To produce EIT images from the captured frames, the process of image reconstruction is applied. Reconstruction algorithms try to solve the problem that is the reverse of EIT, which is the reconstruction of the conductivity distribution within the thorax based upon the voltage measurements collected at electrodes on the thorax’s surface. At first, EIT reconstruction assumed that electrodes were placed on an ellipsoid or circular plane. Newer methods make use of information regarding the anatomical contour of the thorax. In the present, the Sheffield back-projection algorithm as well as the finite-element method (FEM) with a linearized Newton–Raphson algorithm ], and the Graz consensus reconstruction algorithm for EIT (GREIT) [10is frequently employed.
In general, EIT images can be compared to a computed two-dimensional (CT) image: these images are normally rendered so that the viewer is looking from caudal to cranial when reviewing the image. In contrast to the CT image one can observe that an EIT image does not display the appearance of a “slice” but an “EIT sensitivity region” [1111. The EIT sensitive region is a lens-shaped intra-thoracic area that is the source of impedance variations which contribute to the EIT imaging process [11The EIT image is generated by impedance changes. The shape and the thickness of the EIT sensitivity region are dependent on the dimensions, the bioelectric characteristics, and the contour of the thorax as depending on the current injection and voltage measurement pattern [12It is important to note that the shape of the thoracic thorax can.
Time-difference imaging is a technique which is employed for EIT reconstruction to show variations in conductivity, not pure conductivity amounts. In a time-difference EIT image compares the changes in impedance to a base frame. This is a great way to track the time-dependent physiological changes such as respiratory ventilation and perfusion [2]. The color-coding used in EIT images is not uniform but commonly displays the change in impedance to the reference level (2). EIT images are usually colored using a rainbow color scheme with red representing the high relative impedance (e.g. when inspiration occurs) and green representing a medium relative impedance and blue the least relative impedance (e.g. during expiration). In clinical settings, an interesting option is to utilize color scales that range from black (no change in impedance) and blue (intermediate impedance changes) and white (strong impedance change) to code ventilation or from black to white, and white to reflect perfusion.
2. There are a variety of color codes available for EIT images when compared with the CT scan. The rainbow-color scheme utilizes red for the highest absolute impedance (e.g., during inspiration) and green for a intermediate relative impedance, and blue is the color that has the lowest relative intensity (e.g. when expiration is in progress). A more recent color scale uses instead of black (which has no impedance changes), blue for an intermediate impedance shift, and white for the strongest impedance changes.
4. Functional Imaging and EIT Waveform Analysis
Analyzing Impedance Analyzers data is done using EIT waveforms , which are generated in each image’s pixels a series of raw EIT images over long periods of (Figure 3.). Region of Interest (ROI) can be defined to describe activity in the individual pixels in the image. Within any ROI, the waveform shows changes in the region’s conductivity over the course of time that result from respiration (ventilation-related signal, VRS) or cardiac activity (cardiac-related signal, CRS). Additionally, electrically conducting contrast agents such as hypertonic saline can be used in the production of an EIT waveform (indicator-based signal IBS) and is linked to lung perfusion. The CRS can originate from both the cardiac and lung region, and is possibly related to lung perfusion. The exact nature and origin aren’t understood completely 13]. Frequency spectrum analysis is often used to discriminate between ventilationor cardiac-related changes in the impedance. Impedance fluctuations that are not frequent can be caused by adjustments in the ventilation settings.
Figure 3. EIT form and function EIT (fEIT) photographs are derived from raw EIT images. EIT waves can be defined in a pixel-wise manner or based on a specific region in interest (ROI). Conductivity changes occur naturally as a result of ventilatory (VRS) (or cardiac activity (CRS) however they could also be created artificially, e.g. using the injection of bolus (IBS) for perfusion measurements. Images of fEIT show regional physiological parameters including ventilation (V) and perfusion (Q) which are extracted from raw EIT images by using an algorithmic operation over time.
Functional EIT (fEIT) images are generated using a mathematical process on the raw images and the corresponding EIT Waveforms. Since the mathematical operation is applied to determine a physiologically relevant parameter for every pixel, the regional physiological aspects like regional ventilation (V) and respiratory system compliance, as well as regional perfusion (Q) are measured as well as displayed (Figure 3.). Data from EIT waveforms and concurrently recorded airway pressure measurements can be used to calculate the lung compliance and lung closing and opening times for each pixel through changes in pressure and impedance (volume). Similar EIT measurements of the deflation and inflation of lung volumes allow for the display of volume-pressure curves at a pixel level. Depending on the mathematical operation various types of fEIT pictures could address different functional properties from the cardio-pulmonary apparatus.


